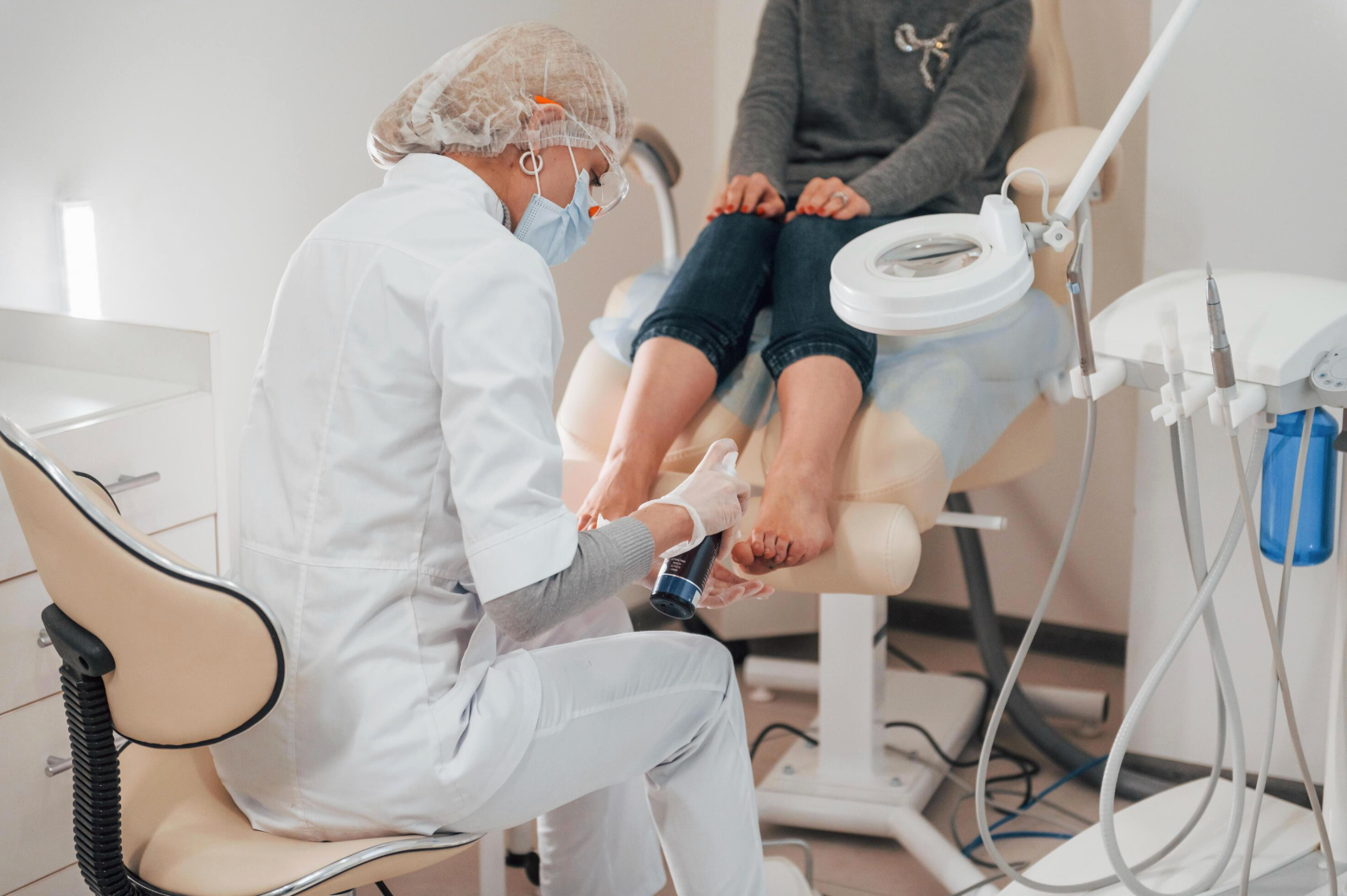
At the chair
Documentation in. Clean claim out.
Refract's AI reads your encounter notes the moment they're signed, pairing class findings, Q-modifiers, and LCD-aligned diagnoses before a claim is ever scrubbed. The chair side stays focused on the patient.